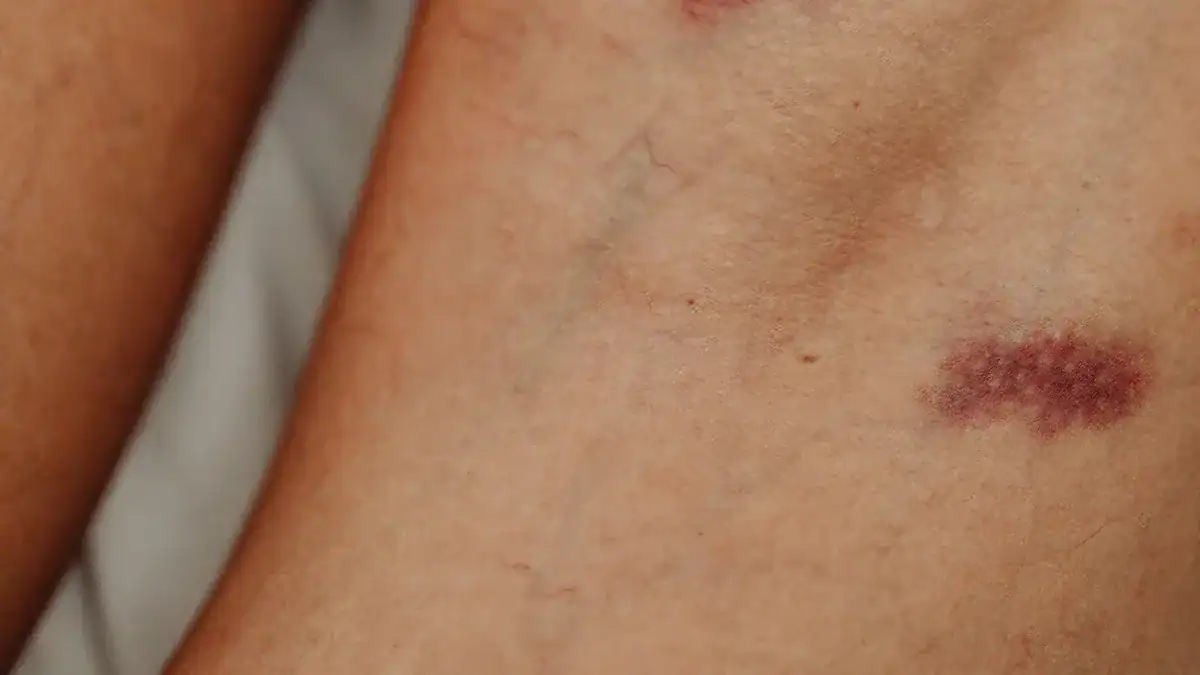
Lower leg redness is a common symptom. Many conditions can cause it, from minor issues to serious ones. You often see this discoloration on your lower leg. It frequently comes with other signs like swelling, pain, or warmth. Your legs might also feel swollen. Understanding these causes helps you get timely and effective treatment.
Key Takeaways
- Many things can make your lower legs red. These include skin infections, poor blood flow, and allergic reactions.
- Look for other signs like swelling, pain, or warmth. These signs help you know what might be wrong.
- See a doctor if redness spreads or you feel sick. Early help can stop problems from getting worse.
- You can help red legs at home. Lift your legs, use cool cloths, and wear special stockings if your doctor says so.
Causes of Lower Leg Redness
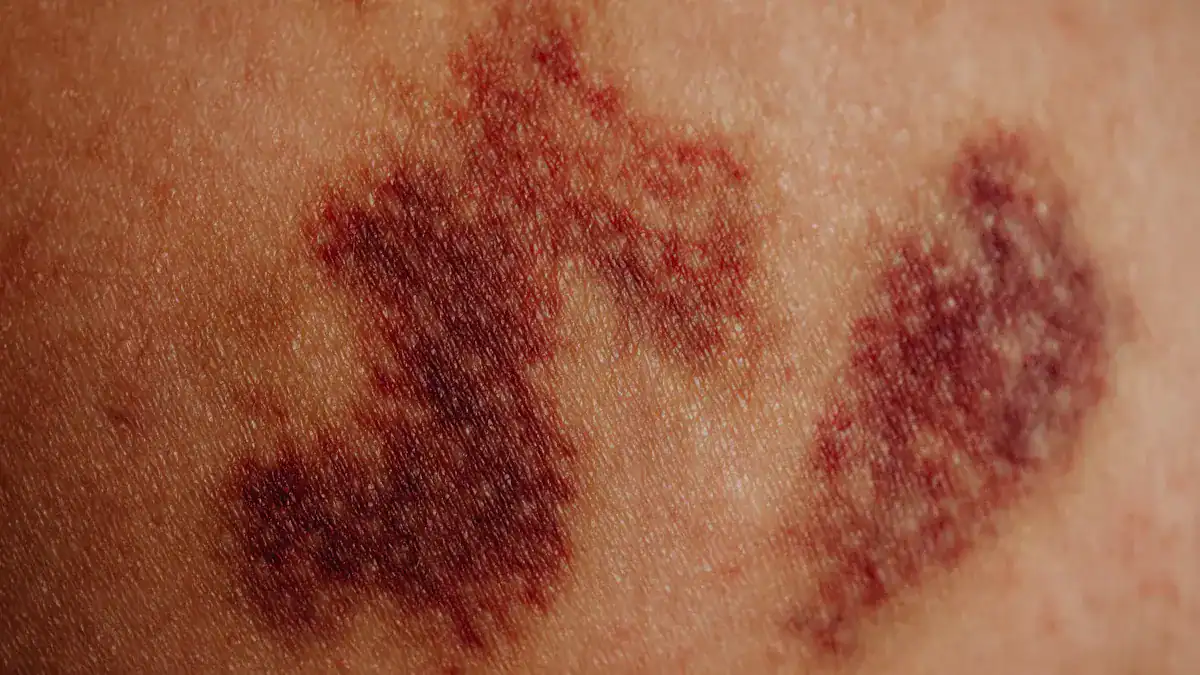
Many different conditions can make your lower legs appear red. These causes range from common skin problems to more serious issues with your blood vessels or immune system. Understanding these causes helps you know what might be happening with your body.
Skin Conditions
Your skin is the body’s largest organ, and many problems with it can cause redness on your legs. One common and serious cause is cellulitis. This is a bacterial infection that gets into your skin through a break, like a cut or scratch. When you have cellulitis, your skin becomes painful, swollen, and feels hot to the touch. The redness spreads quickly.
On lighter skin tones, it looks red or pink. On darker skin, it might appear brown, gray, or purple. This condition needs quick medical care. Another type of leg cellulitis is erysipelas, a bacterial infection in the superficial skin layers. It often has well-defined red edges and can cause blisters.
Venous stasis dermatitis is another frequent cause of lower leg redness, especially for people over 50. This condition affects millions. It happens when your legs swell, putting pressure on your skin. This leads to redness, itching, and a heavy or achy feeling in your legs. You might also see patchy, red, itchy, and scaly skin with blisters. This is also known as gravitational or venous eczema.
Other skin conditions can also cause redness. These include contact dermatitis, which happens when your skin touches something irritating. You might see redness only where the allergen touched your skin. Lipodermatosclerosis is a chronic inflammation that can make your legs look like a “champagne bottle” shape, often with brown staining. Psoriasis and lichen planus are also conditions that can cause red patches on your legs. Folliculitis and tinea corporis are other infections that can cause redness on your legs.
Vascular Problems
Problems with your blood vessels can also lead to redness in your legs. These issues often involve blood flow. Your legs might look red, feel hot, or appear swollen.
Deep vein thrombosis (DVT) is a serious condition where a blood clot forms in a deep vein, usually in your legs. This often causes red skin in the affected leg. Superficial thrombophlebitis involves inflammation of a vein closer to the skin surface, also causing red skin around the inflamed area. May-Thurner syndrome is another condition that can cause red or discolored skin in your leg due to a vein blockage. While less common for widespread redness, Raynaud’s phenomenon can cause color changes, including redness, in your fingers and toes, and sometimes other areas.
Inflammatory & Autoimmune Causes
Sometimes, your body’s immune system can mistakenly attack healthy tissues, leading to inflammation and redness. Vasculitis, for example, involves inflammation of your blood vessels, which can show up as red blotchy skin on your legs. Conditions like psoriasis and lichen planus, mentioned earlier, also have inflammatory components that contribute to redness. These are not infections but rather problems with how your immune system functions.
Other Triggers
Certain external factors or medications can also cause redness. For instance, Red Man Syndrome is a reaction to certain medications, most often vancomycin. If you receive this medication too quickly, you might develop a red rash or redness on your skin. This can appear on your legs, as well as your face, neck, and upper body. This reaction is not an infection but a response to the drug. It happens when bacteria are treated with specific antibiotics.
Understanding Lower Leg Redness: Key Conditions
You now know many things can cause redness on your lower leg. Let’s look closer at some specific conditions. These conditions are common or serious. They often lead to lower leg redness.
Cellulitis: A Common Skin Infection
Cellulitis is a common skin infection. It can make your lower leg red. This infection happens when bacteria get into your skin. You might get it through a cut or scratch. When you have cellulitis, you will see a localized area of redness. This redness might be less clear on darker skin tones. Your skin will feel warm, tender, and painful. The redness can appear patchy. Cellulitis typically affects only one side of your body. Your lower leg is the most common place for this infection. Doctors will check your skin for any breaks or wet areas.
Doctors often prescribe antibiotics to treat cellulitis. For example, they might give you dicloxacillin or cephalexin. Other options include trimethoprim with sulfamethoxazole, clindamycin, or doxycycline. Research shows that high-dose cephalexin can work well for cellulitis. It can lead to fewer treatment failures. For children with moderate cellulitis, high-dose oral cephalexin is effective and safe. If you have had leg cellulitis before, a low dose of penicillin can help prevent it from coming back. This is a cost-effective way to stop future infections.
Venous Stasis Dermatitis
Venous stasis dermatitis is another common cause of lower leg redness. This condition happens when blood does not flow well in your legs. You might notice ankle swelling. Your skin can show orange-brown speckles of discoloration. These are like cayenne pepper spots from tiny burst blood vessels. On lighter skin, you see redness. On darker skin, it might look brown, purple, gray, or ashen. You will likely feel itching, scaling, and dryness. Your legs might feel heavy or achy after standing or sitting for a long time.
If you do not treat it, the swelling can spread to your calf. Your skin might become shiny. You could get open sores, called venous ulcers, on your lower leg and the tops of your feet. These sores can bleed, ooze, and leave scars.
In severe cases, your skin can change permanently. It might become thick, hard, dark, or bumpy, like a cobblestone. You might also feel pain. Your legs can feel heavy or ache when you stand or walk. Swelling often gets worse during the day. It usually gets better after you sleep. Without treatment, your skin can become deeply pigmented and scaly. It can also harden. Your lower calf might even shrink, making your leg look like an upside-down bowling pin. This is called lipodermatosclerosis.
Venous stasis dermatitis is often a chronic condition. You will need long-term care. You can use bland topical moisturizers, like plain white petrolatum, to keep your skin moist. This helps your skin heal. Healing depends on treating the main cause of the problem. Preventing complications is important for your long-term health.
Edema and Swollen Legs and Ankles
Edema means you have too much fluid in your body tissues. This often causes swollen legs and ankles. Many things can cause this fluid retention. For example, standing or sitting for too long can make fluid collect in your lower legs. Eating too much salty food makes your body hold onto water. Certain medicines, like blood pressure drugs or steroids, can also cause edema. Pregnancy often leads to swollen ankles. Obesity can put pressure on your leg veins, causing fluid to build up. Varicose veins and poor blood flow can also cause fluid to collect in your feet and legs. Infections and skin ulcers, especially if you have diabetes, can make areas swollen.
Serious health problems can also cause edema. Heart failure means your heart cannot pump blood well. This leads to fluid buildup and swollen legs and ankles. Liver disease can cause swelling because your liver does not make enough protein to keep fluid in your blood vessels. Kidney damage can stop your body from filtering waste. This causes waste to build up in your lower legs, feet, and ankles.
If you have swollen legs and ankles, your doctor might do some tests. They might check your blood for things like BNP, creatinine, or liver enzymes. These tests help find problems with your heart, kidneys, or liver. They might also check for D-dimer to rule out a blood clot. Imaging tests like venous ultrasonography can check for blood clots or poor blood flow. An echocardiogram can check your heart function. These tests help doctors find the cause of your edema. This helps them treat your swollen legs and ankles.
Other Dermatitis Types
Other types of dermatitis can also cause lower leg redness. Contact dermatitis is one example. This happens when your skin touches something irritating or an allergen. You might see redness only where the substance touched your skin.
Many things can cause contact dermatitis. Common irritants include cement, hair dyes, or long exposure to wet diapers. Pesticides, rubber gloves, and some shampoos can also irritate your skin. Common allergens include adhesives, antibiotics like neomycin, and fragrances in personal products. Metals like nickel, rubber products, and preservatives are also common allergens. Plants like poison ivy can cause a red blotchy skin reaction. Your doctor can help you find out what causes your reaction.
Symptoms and When to Seek Help
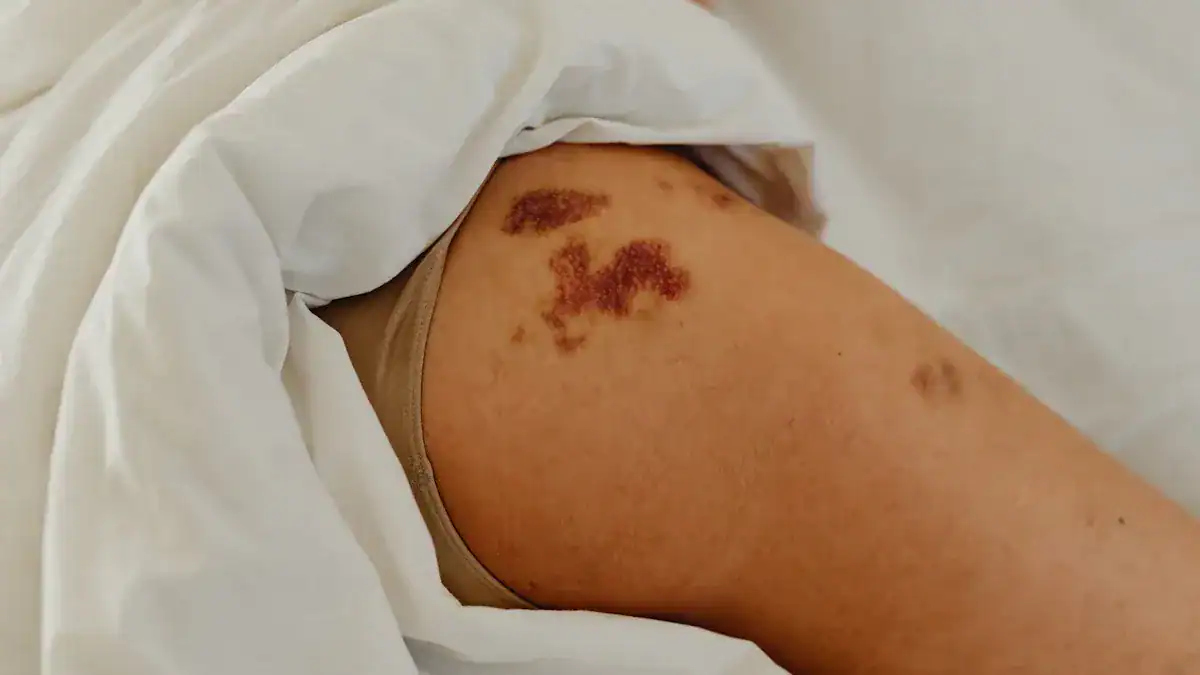
You need to recognize the signs that come with lower leg redness. These accompanying symptoms help you understand what might be happening. Knowing when to seek medical care is also very important.
Accompanying Symptoms
Lower leg redness often comes with other signs. For example, if you have cellulitis, you might notice new or spreading redness. Your skin might also show discoloration. You will feel new or increased swelling, pain, or tenderness. The area will feel hot or burning. You might also feel generally unwell, like you have the flu. These symptoms can start days before other signs appear.
If you have stasis dermatitis, your lower leg redness can come with itching. You might see red, dry, scaly bumps or patches. Your skin can look shiny. You may also notice reddish-brown patches and edema (swelling). In severe cases, you might have oozing, crusted areas, and ulcers.
When a venous leg ulcer causes your lower leg redness, you might also have swollen ankles. The skin around the ulcer can darken. The skin might also feel hard. You may feel a heavy sensation in your legs. Aching or swelling in your legs is common. You might also see red, flaky, scaly, and itchy skin on your legs. Swollen and enlarged veins, called varicose veins, can also be present.
When to Seek Medical Care
You should seek medical care if you notice certain symptoms. If you have leg pain with swelling, redness, or warmth in your calf, see a doctor. Leg pain that occurs with a fever also needs attention. If you have leg cramps with swelling, pain, warmth, and tenderness, get medical help. Swelling, warmth, or skin discoloration along with leg pain can mean you have a blood clot.
Delaying medical help for worsening lower leg redness can cause problems. Earlier diagnosis often leads to faster healing. Delays can make healing times longer. If a wound does not improve, a delayed consultation can happen in an emergency setting. This might prevent a full assessment. This can make outcomes worse. For example, untreated cellulitis can lead to serious complications.
Diagnostic delays are common for unusual wounds. These include cancers or certain skin conditions. A delayed diagnosis of Charcot’s foot can also worsen patient outcomes. More than half of these cases have a delay from when symptoms start to when doctors find the correct diagnosis.
| Diagnostic Delay | Odds Ratio (0.18–0.52) |
|---|---|
| Less than 4 weeks | Ref |
| Between 4 and 12 weeks | 0.31 |
| Over 12 weeks | 0.17 |
Treatment Options for Lower Leg Redness
You have many ways to manage and treat lower leg redness. The best approach depends on what causes your redness. You can use home care, medical treatments, and lifestyle changes.
Home Care Strategies
You can manage mild lower leg redness at home. Elevating your legs helps blood flow. It reduces swelling. Cool compresses bring relief from redness and discomfort. Wear compression stockings. They support blood flow. This is especially true for chronic venous insufficiency. You can use over-the-counter anti-inflammatory medicines.
Antihistamines also help manage symptoms. Apply anti-inflammatory creams. Use antihistamines for allergic reactions. Moisturizers help dry skin. Keep good hygiene. Avoid things that irritate your skin.
Keep your skin moisturized. Wear loose-fitting clothing. Stay active. Avoid sitting or standing too long if you have circulation issues. Exercise regularly. This improves circulation. It reduces the risk of red areas.
Avoid over-exertion or injury. Maintain a healthy weight. Engage in consistent physical activity. Avoid tight clothes. They can stop blood flow. Wear compression stockings if your doctor recommends them. Moisturize regularly.
Compression stockings are very helpful. Doctors prefer them for ongoing swelling. They give continuous support all day. Elevating your lower limbs only helps for a short time. Studies show compression therapy works. Stockings with 22 mmHg pressure or higher greatly reduce leg swelling.
This helps with swollen legs and ankles. Stronger compression gives better results. Compression stockings do more than reduce swelling. They ease leg pain and tiredness from varicose veins. Patients report less pain and swelling. Their quality of life improves.
Compression stockings fix the cause of venous swelling. They strengthen vein walls. They improve circulation. This stops fluid from pooling. This fluid retention can cause edema.
Elevating your lower limbs only drains fluid already there. Elevation and massage can help. But compression therapy is the main way to stop daily swelling. This helps prevent swollen legs and ankles from recurring.
Prevention & Lifestyle
You can prevent future episodes of lower leg redness. Avoid standing or sitting for long times. Elevate your feet when you sit. Wear compression stockings. Choose loose-fitting clothes. This prevents skin irritation. Treat underlying conditions. These include high blood pressure or congestive heart failure.
They can cause venous insufficiency. Eating balanced meals helps. Get enough vitamins A, C, zinc, and protein. Stay hydrated. This boosts circulation. Exercise regularly. Walking improves leg circulation. Practice good foot care. Use compression stockings. Avoid long periods of standing or sitting.
Manage chronic conditions like diabetes. This helps prevent swollen legs and ankles. Go for regular health check-ups. This helps find problems early. Good hygiene also helps prevent bacteria from causing issues around your ankles. This comprehensive approach is key to long-term treatment and prevention of swollen lower legs and ankles. Reducing edema in your legs is a key goal.
Lower leg redness is a symptom that needs your attention. It has many different causes. You must observe any other symptoms you have. This helps you understand when to see a healthcare professional for a correct diagnosis.
Early intervention prevents complications and leads to better outcomes. Untreated issues can cause serious problems. You risk bone infections, severe cellulitis, sepsis, or even skin cancers like squamous cell carcinoma. With prompt treatment, small patches of cellulitis often improve in about a week.
However, you might still have swelling or discomfort for longer. This is normal and does not mean treatment failed. Always seek medical advice for persistent, worsening, or concerning lower leg redness.

