
A cardiologist is a medical doctor. This heart specialist assesses, diagnoses, and treats issues related to the heart and blood vessels.
The heart is a complex organ, requiring specialized expertise for various conditions and treatments. Globally, cardiovascular disease cases more than doubled from 1990 to 2023, reaching 626 million. In the United States, heart disease remains the leading cause of death. This highlights the critical need for different types of cardiologists. Understanding these specializations helps patients navigate their healthcare journey more effectively and find the essential heart specialist for their needs within the field of cardiology.
Key Takeaways
General cardiologists are the first doctors for heart problems. They diagnose common heart issues and manage them with medicine or lifestyle changes.
Interventional cardiologists fix heart problems with small tubes. They can open blocked arteries and repair heart valves without big surgery.
Electrophysiologists treat heart rhythm problems. They use special tools to check the heart’s electrical system and fix irregular heartbeats.
Cardio-oncologists help cancer patients keep their hearts healthy. They manage heart issues that can happen because of cancer treatments.
Pediatric cardiologists care for children’s hearts. They treat heart problems that babies are born with and help children as they grow.
General Cardiologists: Understanding the Core Types of Cardiologists

General cardiologists serve as the primary point of contact for most heart-related concerns. They act as the “first line of defense” in diagnosing and managing various cardiovascular conditions. This type of cardiologist provides comprehensive care, guiding patients through initial assessments and treatment plans.
Initial Diagnosis and Management
A general cardiologist performs initial evaluations. They assess symptoms, review medical history, and conduct physical examinations. Patients often see a general cardiologist for common issues. These include chest complaints, which account for about 44% of referrals. Palpitations are another frequent reason, making up 19% of cases.
Dyspnoea, or shortness of breath, represents 12% of referrals. Other reasons include sudden loss of consciousness, abnormal ECG results, screening for cardiac disease, heart murmurs, preoperative screening, and identifying the cardiac origin of emboli. The general cardiologist then develops a management strategy. This strategy may involve lifestyle changes, medication, or further specialized testing.
Common Heart Conditions
General cardiologists manage a wide range of common heart conditions. They treat high blood pressure, high cholesterol, and coronary artery disease. They also address early stages of heart failure and arrhythmias. Their expertise helps patients understand their condition and follow effective treatment plans. They monitor patient progress and adjust treatments as needed.
Non-Invasive Procedures
General cardiologists frequently use non-invasive diagnostic procedures. These tests help them understand the heart’s function without surgery. Common procedures include electrocardiograms (ECG/EKG), which capture the heart’s electrical activity.
Echocardiography uses ultrasound waves to create detailed images of the heart. This assesses blood pumping, infections, and structural issues. Other tools include X-rays, stress tests, and Holter monitors.
Stress tests evaluate heart performance under physical stress. Holter monitors record the heart’s electrical activity over time. Cardiac CT scans and MRI also provide images for examining heart disease and atherosclerosis. Nuclear cardiology uses radioactive elements to study cardiovascular disorders. These tools help the general cardiologist make accurate diagnoses and plan appropriate care. They are an essential heart specialist for foundational cardiac health.
Interventional Cardiologists
Interventional cardiologists specialize in minimally invasive, catheter-based procedures. They use thin, flexible tubes called catheters to diagnose and treat various heart conditions. This specialized area of cardiology helps patients avoid more invasive open-heart surgery.
Catheter-Based Treatments
Interventional cardiologists perform many catheter-based treatments. They use Percutaneous Coronary Intervention (PCI), which includes angioplasty and stent placement, to open blocked arteries. They also perform Transcatheter Aortic Valve Replacement (TAVR) for damaged aortic valves.
Other procedures include closing holes in the heart, such as Atrial Septal Defect (ASD) and Patent Foramen Ovale (PFO) closures. They also treat peripheral arterial disease with angioplasty and stent placement in the limbs. These specialists can also implant and extract Inferior Vena Cava (IVC) filters. They use intravascular ultrasound to get internal images of the heart.
Conditions Requiring Intervention
Several heart conditions often require intervention from this type of cardiologist. Arteries clogged with plaque are a common issue.
Damaged heart valves, especially aortic valves, also need treatment. Adult congenital heart disease, which involves heart defects present from birth, frequently requires interventional services. Cardiac arrest and heart attacks demand emergency interventional procedures. Structural heart disease, which includes various defects in the heart’s structure, also falls under their care. For example, a patent foramen ovale, an opening between the heart’s upper chambers, can be closed using catheter-based techniques.
Key Interventional Procedures
Angioplasty and stenting are key interventional procedures, especially for coronary artery disease. During angioplasty, a catheter guides a tiny balloon to a blocked artery. The balloon inflates to widen the artery.
Then, a mesh stent is often placed to keep the artery open and prevent re-narrowing. This procedure is crucial for heart attacks and also opens narrowed arteries in non-emergency situations. Interventional cardiologists also perform complex coronary angioplasty and stenting for severe blockages. They are an essential heart specialist for patients needing these advanced, minimally invasive treatments.
Electrophysiologists
Electrophysiologists are specialized doctors within cardiology. They focus on the heart’s electrical system. These experts diagnose and treat heart rhythm disorders, also known as arrhythmias. They understand how electrical signals control heartbeats.
Heart Rhythm Disorders
Heart rhythm disorders occur when the heart beats too fast, too slow, or irregularly. Atrial fibrillation (A-Fib) is the most common chronic heart rhythm disorder in adults. It affects millions globally. A-Fib causes disorganized, rapid, and irregular beating in the heart’s upper chambers. Other common rhythm disorders include:
Atrial Flutter
Heart Block
Ventricular Tachycardia
Sick Sinus Syndrome
Supraventricular Tachycardia
The prevalence of heart rhythm abnormalities increases with age. Males generally show a higher prevalence than females across all age groups.
Age Group | Males (Any rhythm abnormality) | Females (Any rhythm abnormality) |
|---|---|---|
< 55 years | 1.28% | 0.70% |
55 to 64 years | 3.62% | 1.57% |
≥ 65 years | 6.56% | 3.17% |
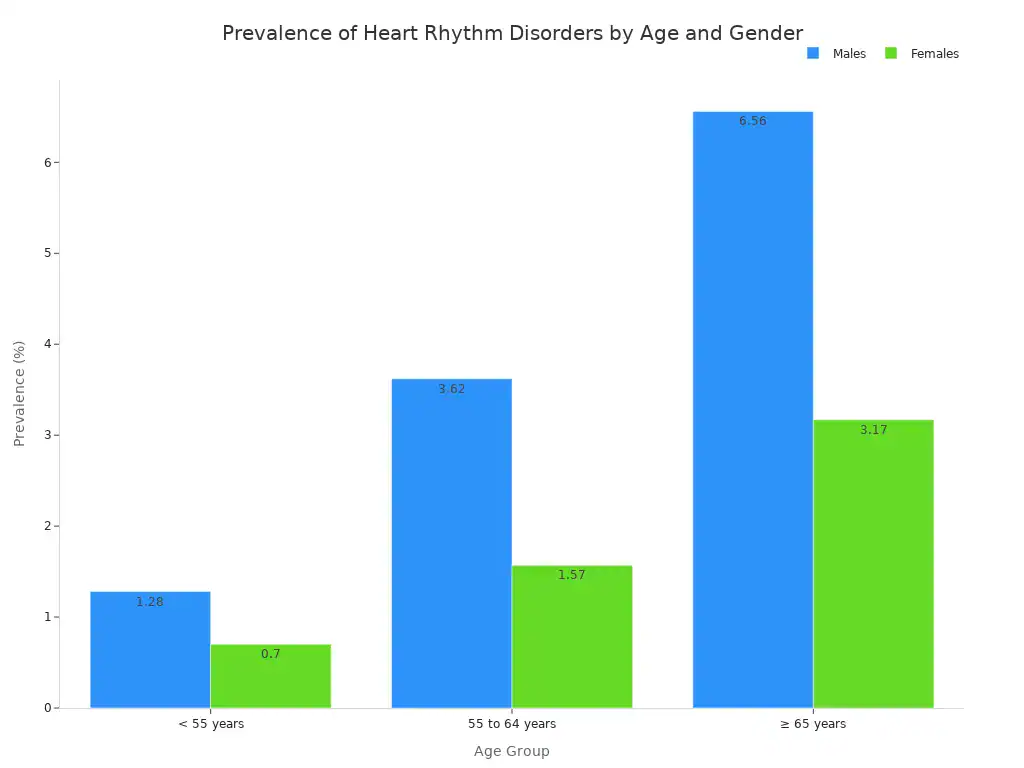
Overall, about 2.15% of the population experiences a clinically relevant rhythm abnormality.
Electrical System Assessment
Electrophysiologists use various tools to assess the heart’s electrical system. An electrocardiogram (EKG or ECG) records the heart’s electrical activity. Different types of EKG devices exist:
Standard 12-lead EKG: Doctors use this in their office.
Holter monitor: Patients wear this for 24 to 48 hours for continuous recording.
Event monitor: Patients wear this for a week or more, recording when symptoms occur.
Implanted loop recorder: Doctors place this under the skin for several years.
Stress test EKG: Doctors take readings while a patient exercises.
These devices help identify the specific type and origin of an arrhythmia.
Arrhythmia Procedures
Electrophysiologists perform specialized procedures to correct heart rhythm problems. These include:
Cardiac Ablation: This procedure uses heat or radiofrequency energy. It eliminates abnormal heart tissue causing arrhythmias.
Pacemaker Implantation: Doctors insert a device to monitor and regulate heart rate with electrical impulses.
Defibrillator Implantation: This device continuously monitors the heart. It delivers a life-saving electrical shock for dangerous irregular heartbeats.
DC Cardioversion: This uses a controlled electrical shock to reset the heart’s rhythm.
Electrophysiology Study (EPS): This diagnostic procedure uses electrodes to record heart’s electrical signals. It helps identify arrhythmia sources.
These interventions help patients achieve a normal heart rhythm and improve their quality of life.
Heart Failure Specialists
Heart failure specialists manage advanced heart conditions. They focus on comprehensive care for weakened hearts. This type of cardiologist helps patients with severe heart failure navigate complex treatment paths.
Advanced Heart Care
Many treatment options are available for advanced heart failure. The Heart Association offers recommendations for aggressive treatment versus comfort care. These options include extracorporeal membrane oxygenation, heart transplantation, and ventricular assist devices.
Other advanced therapies for severe heart failure include total artificial hearts and the CardioMEMS™ Heart Failure (HF) System. Without life-prolonging therapies like LVAD and heart transplant, half of advanced heart failure patients die within one year. Only about one-quarter survive more than two years. For selected patients with heart failure treated with advanced therapies, such as intravenous inotropes for palliation, survival can be over 50% at one year. Patients receiving LVADs or a heart transplant can extend their life expectancy well beyond 5-10 years.
Management Strategies
Heart failure specialists employ various strategies to manage heart failure. These include pharmacological agents, device-based therapies, and lifestyle modifications.
Pharmacological Agents:
ACE inhibitors (e.g., enalapril)
ARBs (e.g., valsartan)
Beta-blockers (e.g., carvedilol)
Mineralocorticoid receptor antagonists (e.g., spironolactone)
Sacubitril/valsartan (ARNI)
Diuretics (e.g., furosemide)
Digoxin
Ivabradine
Device-Based Therapies:
Implantable Cardioverter-Defibrillators (ICDs)
Cardiac Resynchronization Therapy (CRT)
Left Ventricular Assist Devices (LVADs)
Lifestyle changes also play a crucial role in managing heart failure. These include dietary sodium restriction, fluid restriction, weight management, and regular exercise. Smoking cessation and alcohol restriction are also vital. Heart transplantation is the ultimate therapy for end-stage heart failure when other treatments are no longer effective.
Improving Quality of Life
Heart failure specialists significantly improve patients’ quality of life. They integrate palliative care into treatment plans. Palliative care focuses on relieving symptoms and stress from serious illnesses like heart failure.
It aims to improve quality of life for both the patient and their family. Palliative care teams manage symptoms, side effects, and stresses. They reduce fluid buildup, swelling, and pain. They also help patients understand their unpredictable condition and cope with daily challenges. Specialists advocate for a ‘both/and’ model. This combines life-prolonging treatments with palliative care. This approach enhances quality of life and daily functioning simultaneously for patients with heart failure.
Palliative care, which is medical help to relieve the symptoms and stress of a serious illness, should be an integral part of the treatment plan for heart failure patients. Research indicates that palliative care can significantly improve quality of life and symptom control, addressing issues such as depression, anxiety, and social withdrawal.
Cardio-Oncologists: An Essential Heart Specialist Role
Cardio-oncologists represent a specialized field within cardiology. This essential heart specialist addresses heart issues in cancer patients. They specifically manage the cardiovascular side effects of cancer treatments. A cardio-oncologist ensures patients receive optimal cancer care while protecting their heart health.
Preventing Cardiac Complications
Cardio-oncologists employ several strategies to prevent cardiac complications in cancer patients. They use risk stratification to identify patients at higher risk for cancer therapy-related cardiac dysfunction (CTRCD). These patients require closer cardiologic surveillance.
Cardioprotective approaches, both pharmacological and non-pharmacological, reduce CTRCD risk after cancer therapy begins. Early detection through highly sensitive non-invasive cardiologic diagnostic tools allows for timely adjustments to cancer therapy.
This also initiates treatment to prevent progression. Lifestyle optimization, including smoking cessation and alcohol restriction, plays a vital role. Intensive management of cardiovascular risk factors like hypertension, diabetes, and dyslipidemia is crucial. Regular exercise improves cardiorespiratory fitness. This links to lower rates of CTRCD or cardiovascular events in some studies. Genetic testing shows promise for preventing CTRCD, but doctors do not yet routinely recommend it.
Pediatric Cardiologists
Pediatric cardiologists care for young hearts. They address heart defects present from birth and provide ongoing care for children. These specialists understand the unique needs of growing bodies and developing hearts.
Congenital Heart Conditions
Congenital heart disease (CHD) refers to heart problems present at birth. These conditions affect the heart’s structure or function. The incidence of CHD varies across studies. It ranges from about 4 to 50 per 1,000 live births. If doctors include conditions like bicuspid aortic valves or a silent patent ductus arteriosus, this number can increase to 20 per 1,000 live births. Moderate and severe forms of CHD occur in about 6 per 1,000 live births. Globally, experts often cite CHD incidence as 8 per 1,000 live births, with some recent studies showing it as high as 9.5 per 1,000.
Common congenital heart conditions include:
Atrial Septal Defect (ASD)
Ventricular Septal Defect
Coarctation of the Aorta (CoA)
Tetralogy of Fallot
Hypoplastic Left Heart Syndrome (HLHS)
Pulmonary Stenosis (PS)
Transposition of the Great Arteries
Specialized Care for Children
Pediatric cardiologists offer specialized care tailored to children. They diagnose heart conditions in fetuses, infants, children, and adolescents. Their treatment plans consider a child’s growth and development. They use child-friendly diagnostic tools and procedures. This ensures comfort and accuracy. They also work closely with families, providing support and education. This comprehensive approach helps children manage their heart conditions throughout their lives.
Developmental Heart Issues
Children with heart conditions sometimes face developmental challenges. Studies show children born with symptomatic congenital heart defects have a higher risk of adverse neurodevelopmental outcomes by 8 years of age. This risk is greatest for those who experienced both cyanosis (blue skin due to lack of oxygen) and heart failure at birth. Researchers have investigated predictors of developmental disabilities after heart surgery in young children. They also explored how long a hospital stay after infant heart surgery relates to cognitive outcomes later in life.
Children with certain heart conditions may show differences in cognitive scores:
Group | IQ Score Difference (95% CI) | Language Score Difference (95% CI) | Memory and Learning Score Difference (95% CI) |
|---|---|---|---|
Cyanotic CHD without Heart Failure | -7.2 (-13.4 to -1.2) | N/A | N/A |
Noncyanotic CHD with Heart Failure | N/A | -1.5 (-2.2 to -0.7) | -1.3 (-2.4 to -0.3) |
Cyanotic CHD with Heart Failure | -7.6 (-13.5 to -1.8) | -2.0 (-2.9 to -1.0) | -1.1 (-2.3 to -0.1) |
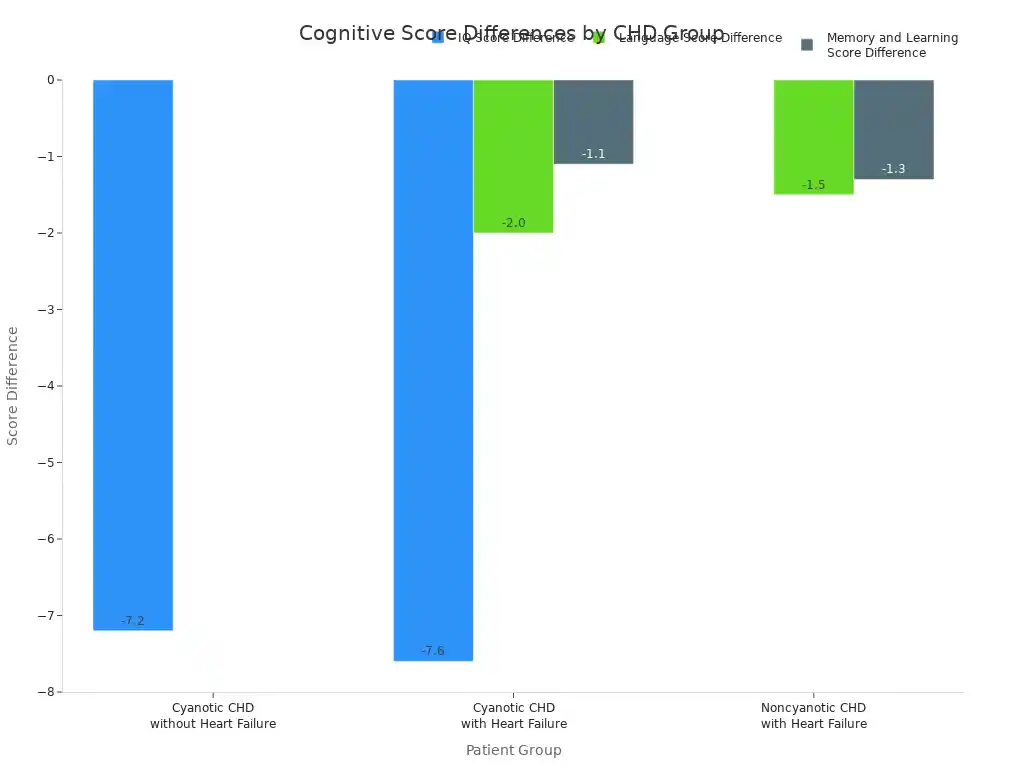
These findings highlight the importance of ongoing monitoring and support for children with heart conditions. Pediatric cardiology plays a vital role in addressing these complex needs.
Specialized cardiac care is crucial for heart health. Each type of cardiologist, from general to pediatric, plays a vital role. The right essential heart specialist significantly impacts diagnosis, treatment, and long-term outcomes. For example, studies show cardiac intensivists reduce in-hospital mortality rates.
Variable | Odds Ratio (OR) | 95% Confidence Interval (CI) | p-value |
|---|---|---|---|
Cardiac intensivists | 0.474 | 0.311–0.725 | 0.001 |
Age (per 1 year) | 1.031 | 1.015–1.047 | < 0.001 |
CKD | 2.817 | 1.601–4.957 | < 0.001 |
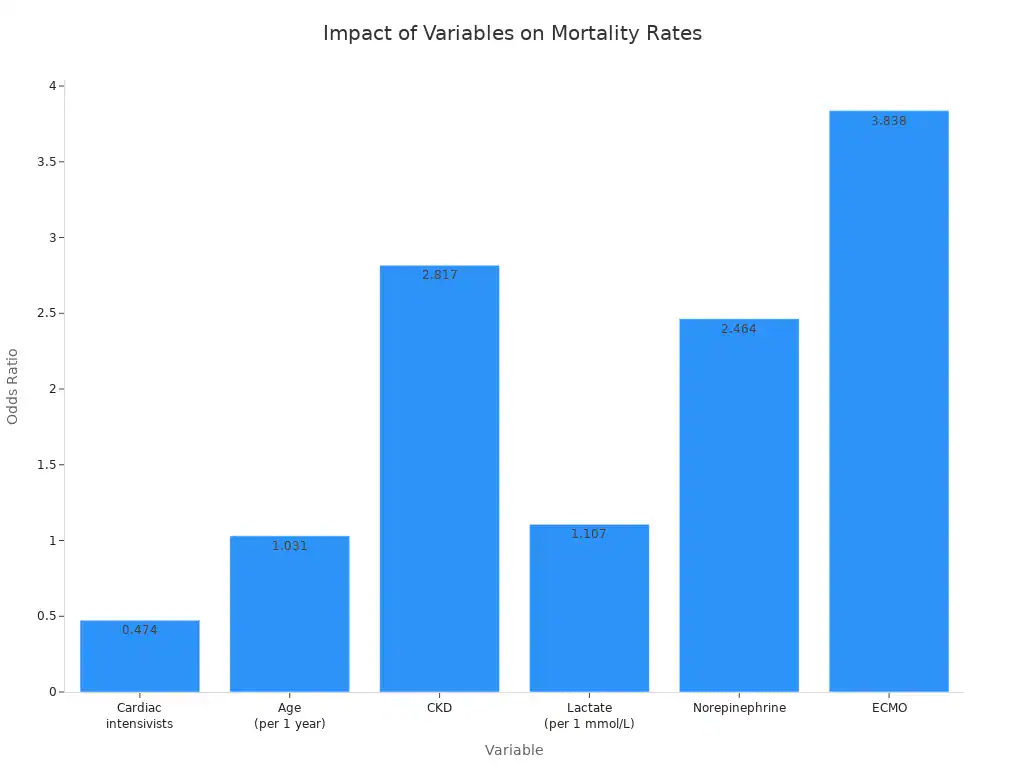
This specialized management improves patient survival. Readers should consult their primary care physician. This helps determine the most appropriate cardiologist for their needs. Proactive heart health management and expert medical advice are essential in cardiology. This ensures better outcomes in cardiology.
FAQ
What is a general cardiologist’s primary role?
A general cardiologist serves as the first contact for heart concerns. They diagnose and manage common heart conditions. They also perform non-invasive tests like EKGs and echocardiograms. This specialist guides patients through initial assessments and treatment plans.


